
Meperidine, also known as Pethidine, is an artificially synthesized opioid that is in common use as a strong painkiller. It belongs to the Phenylpiperidines subclass of medications and has similar powerful effects to those of Morphine. The drug is also sold under the brand name Demerol. Demerol drugs, when used as directed by a doctor, have been proven to effectively manage pain without untoward, moderate to severe side effects.
Table Of Contents:
However, chronic use may result in tolerance, meaning that as time passes, chronic users may have to increase their dose to achieve the same effects they did when they started treatment with the medication, which, in its turn, may lead to addiction. Demerol addiction and dependence may also come with long-term use. It must be noted, too, that Demerol abuse, misuse, dependence, and addiction can possibly develop even when it is used or taken as recommended by a health professional, due to its ability to cause tolerance.
The changes in the brain caused by regular drug use can be persistent and may interfere with one’s self-control and ability to resist urges to take the drug, making dealing with Demerol addiction quite a challenge.
More About Opioids:
What is Demerol?
Demerol (generic Meperidine) is an opioid painkiller used for the short-term treatment of moderate to severe pain-related signs (in surgery and labor, etc.). It is classified as a Schedule II controlled substance, more commonly known as dangerous drugs. This means that there is a high risk of Demerol abuse, with individuals using this drug having the potential to develop low to moderate physical dependence or severe psychological dependence. Despite the fact, Meperidine can be obtained with a prescription as it is FDA-approved and has a currently accepted medical use for the treatment of moderate to severe pain. Prescription orders for Schedule II substances such as this drug, however, are subject to restrictions. For one, they must be written and signed by the medical practitioner. They may also not be refilled or telephoned in to the pharmacy, except for emergency cases.

Demerol Dosage Forms and Strengths
Demerol drugs come in different forms: parenteral or Demerol injection, Demerol pill or tablet, and oral solution.
Demerol injection comes in Carpuject single-dose cartridge, Uni-Amp unit dose pak-ampuls, and multiple-dose vials:
- The Carpuject single-dose cartridge comes in the 4 strengths: 25mg/mL, 50mg/mL, 75 mg/mL, and 100mg/mL.
- The Uni-Amp unit dose pak-ampuls, on the other hand, comes in 5 strengths: 25mg/0.5mL, 50mg/mL, 75mg/1.5mL, 100mg/mL, and 100mg/2mL.
- Lastly, the Demerol injection multiple-dose vials come in 2 strengths: 1500mg/30mL or 50mg/mL and 2000mg/20mL or 100mg/mL, both of which contain 0.1% metacresol that acts as a preservative.
Meperidine tablets are available in 2 strengths: 50mg and 100mg. They both have a round shape and a convex surface and are white in color.
Demerol drugs are also available in oral solutions. They come in 16 fl. oz bottles in a strength of 50mg/5mL or 10mg/mL. Demerol drugs in this form are alcohol-free and banana-flavored.
Demerol Mechanism of Action
Demerol drugs are agonists to the mu-opioid receptor and weak inhibitors of serotonin transporters – they exhibit serotonergic activity and are linked with serotonin syndrome. Although this medication has several actions similar to those of Morphine (such as sedation), it has a direct, non-opioid receptor mechanism. Meperidine also exhibits a hepatic metabolism by hydrolysis and N-demethylation, and so its principal actions include analgesia. Further, it inhibits voltage-gated Na+ mediated by an opiate drug-receptor and interacts with sodium ion channels, resulting in local anesthetic-like effects. Meanwhile, its post-transcriptional mechanism decreases shivers and chills, and by inhibiting the norepinephrine and dopamine transporters, it produces stimulant effects.
Common Demerol Side Effects
As with other drugs, Meperidine (whether in Demerol pill, oral solution, or injection form) may cause side effects. Most of them are minor and quite common, but there are also severe ones that could be due to long-term use.
Below Are Some of the Most Common Meperidine Side Effects:
- Sedation
- Agitation
- Dizziness
- Passing out
- Lightheadedness
- Nervousness
- Headache
- Vomiting
- Nausea
- Dry mouth
- Sweating
- Flushing
- Extreme calm
- Confusion
- Weakness
- Loss of appetite
- Constipation
- Stomach cramps
- Abdominal pain
- Changes in mood
- Changes in eyesight
- Abnormal heartbeat
- Chest pain
- Low blood pressure
- Restlessness
- Itching
- Hard time urinating
- Trouble breathing
Experiencing side effects from using this medication at the prescribed dose may be rare, but some individuals may have them bad. With this, it’s important to always watch out for them and immediately ask a doctor or health professional for medical help if needed.

Short-Term Demerol Side Effects
People who were under Meperidine treatment for a short time may also experience side effects, although not as severe as long-term side effects.
Some Short-Term Side Effects One May Experience Are:
- Unusual tiredness
- Cognitive problems
- Poor coordination
- Libido issues / decreased interest in sex
- Diarrhea
- Redness, puffiness, or swelling of the face, neck, arms, or upper chest
- Irregular menstrual cycle
- Hives
- Shivering
- Twitching
- Hallucinations
Note that these symptoms may vary in severity from person to person. Getting medical advice about them is highly recommended.
Demerol Long-Term Effects
Side effects and symptoms caused by long-term Meperidine use can be extremely dangerous and may be life-threatening.
Using This Drug for Long May Cause the Following Effects to Develop:
- Neuroleptic malignant syndrome (NMS)
- Serotonin syndrome
- Insufficient oxygenation of blood and tissues or hypoxia
- Brain damage
- Anxiety and depression, among other psychological problems
- Physical dependence
- Addiction
Patients suspected of having any of these should not be left unmonitored. It is best if they seek professional help to mitigate the symptoms they are experiencing.
Abusing Meperidine can lead to overdose and in some cases, death. Patients under treatment with this medication must be assessed carefully and monitored regularly – checking for the development of the behavioral and physical signs of abuse and addiction.
Indication for Demerol Use And Risks of Addiction
One of the most common Demerol uses is relieving moderate to severe pain. Also, because it demonstrates less respiratory depression than other similar drugs while enhancing the effects of anesthesia, another one of Demerol uses can be during or prior to a surgical procedure. It must be noted that there exist Demerol contraindications for patients hypersensitive to Meperidine. There are also Demerol contraindications for patients receiving or who have recently received MAO (monoamine oxidase) inhibitors as well.
As mentioned earlier, like all opiates, there is a high risk for Demerol abuse and misuse. Demerol activates reward regions in one’s brain, reduces anxiety, and immediately decreases physical pain. And so, an analgesic effect of euphoria is also created. For this reason, one may develop substance use disorder over time and the potential for Demerol addiction is increased even in individuals who take their medication as prescribed or advised by the doctor. This is especially true when it is used long-term since it can cause changes in chemical systems and circuits of the brain. When the central nervous system has adapted to the drug, one may have trouble with normal functioning without it. They can develop dependence, tolerance, and eventually harmful compulsive drug-seeking behavior that can lead to Demerol abuse and/or Demerol addiction, which pose a high risk for overdose and death.
The changes in the brain caused by regular drug use can be persistent and may interfere with one’s self-control and ability to resist urges to take the drug, making dealing with Demerol addiction quite a challenge. This increases the risk for relapse extremely common for people recovering from Demerol abuse and addiction, although it doesn’t necessarily eliminate the chances of addiction treatment to work. A recovering individual may experience withdrawal symptoms such as problems with judgment, learning, memory, stress, behavior, and decision-making.
Who Is Most at Risk Of Demerol Addiction?
There is not really an exact indicator or a sure way to assess and determine if a person is more at risk of drug addiction than another, but people with a history of drug abuse are among the population at high risk of addiction to Meperidine. They include:
- Already-drug abusers and addicts (especially those untreated)
- Individuals who have undergone treatment with therapeutic doses as they may have developed tolerance
Individual factors such as biology, environment, and development also influence the risk for addiction. People possessing more risk factors have a greater chance of abusing the drug and becoming addicted to it.
How These Factors Influence Risks Are Further Discussed Below.
- Genetics and the presence of mental disorders or certain diseases could influence one’s risk for drug misuse, abuse, and addiction as gene variations are one of the contributors to one’s level of risk or protection. Risks are also increased for infants whose mothers were opioid-dependent during pregnancy.
- The environment and quality of life of an individual could also have a huge effect on this.
- Early exposure to substance abuse, like in situations where an individual witnesses other people in their household abuse drugs make them more prone to harmful behaviors and abuse.
Peer pressure, stress, and lack of parental guidance especially during one’s critical developmental stages and teenage years also increase the likelihood of drug addiction.

Demerol Abuse Statistics
There are currently no numbers and data of abuse specific to Demerol abuse. However, risks and deaths of opioid abuse are well-documented. In 2017, the HHS (U.S. Department of Health and Human Services) declared a public health emergency in response to the opioid epidemic as deaths involving opioid overdose significantly increased from 1999 to 2019.
Deaths involving opioid overdose amounted to 50000 in 2019 – 6 times the number of deaths in 1999. In 2019, over 36000 people died of synthetic opioid overdose such as Demerol in the United States, as reported by the Centers for Disease Control and Prevention. This death rate is higher than that of 2018’s by over 15% and is over 11 times higher than in 2013.
Signs and Symptoms Of Meperidine Abuse And Addiction
There are several psychological, behavioral, and physical signs and symptoms that may be indicative of Meperidine abuse, overdose, and addiction.
Psychosocial and Behavioral Signs
People with substance abuse and addiction issues frequently exhibit psychosocial and behavioral signs. They often lead to problems in relationships and at home, school, or work.
Some of the Most Common Behavioral Signs Include the Following:
- Sudden mood swings and attitude or personality changes
- Feelings of helplessness, shame, and isolation
- Engagement in suspicious behaviors such as drug-seeking
- Disorientation or spacing out
- Neglect of life responsibilities
- Irritability
- Lack of consciousness and critical mental function
- Hallucination
- Delirium
- Anxiety, feeling of nervousness, or paranoia
- Withdrawal syndrome
- Agitation
- Hyperexcitability
Being aware of these signs is helpful if someone is suspected of Meperidine abuse and addiction. If one or more of these symptoms are present, know that help is available. Recognizing the problem early on is the important first step in recovery.
Physical Signs
Physical effects caused by synthetic opioids are often noticeable. Some effects may be mild in nature, but there are also dangerous and potentially fatal ones.
Physical Effects and Signs May Include:
- Extreme drowsiness
- Dizziness
- Nausea
- Blurred vision
- Decreased appetite
- Generalized tonic-clonic seizures
- Pneumonia
- Apnea
- Circulatory system failure
- Slow heart rate
- Abnormal breathing
- Cardiac/respiratory arrest
- CNS depression
- Coma
- Hypothermia
- Hypotension
- Muscle paralysis
- Weakness
- Larger or smaller pupils
- Pulmonary edema
- Convulsions
- Changes in sleep patterns
Individuals suspected of abuse and/or addiction to Meperidine should be monitored closely. A doctor should regularly check for the symptoms above – the presence of more than one of them could be indicative of misuse, abuse, and addiction.
To avoid potentially life-threatening withdrawal symptoms and for addiction treatment to be successful, the dosage is gradually reduced with the specifics depending on a patient’s physical and psychological attributes.
Possible Dangers of Meperidine Abuse
Abusing Meperidine can lead to overdose and in some cases, death. Patients under treatment with this medication must be assessed carefully and monitored regularly – checking for the development of the behavioral and physical signs mentioned above. Abusing this drug can lead to adverse reactions and dangerous, life-threatening effects. Aside from those previously mentioned, one may also develop serotonin syndrome, a potentially fatal condition. In specific populations such as those with hepatic or renal impairment, abuse can result in excitatory effects in the CNS as well as CNS and respiratory depression. Anyone who is to undergo treatment with this medication should get as much information about the adverse effects they may experience. Using Meperidine should be approached with extreme caution, and regular monitoring both by a physician and their caregiver, family, or other people in the household is strongly advised, especially with patients suspected of abuse with a history of it.
Demerol Overdose
Opioid addicts are at an increased likelihood to overdose on Meperidine, but overdose occurs in absolutely anyone who accidentally or intentionally takes more than the recommended dose of this medication. In Meperidine overdose cases, symptoms could present in different parts of the body.
The Following Are Some of Them:
- Widened pupil
- Decreased/weakened blood pressure/pulse
- Difficulty breathing
- Unresponsiveness
- Unconsciousness
- Sedation
- Fatigue
- Dizziness
- Seizures
- Cardiac arrest
- Respiratory depression
- Low body temperature
- Muscle twitching
- Clammy and itchy skin
- Stomach/intestine spasms
- Constipation
- Vomiting
If someone is suspected of overdose, seek medical help and call an emergency right away. While waiting for help to arrive, gather as much information as it could be of great help in determining the treatment option suitable for them. This includes the individual’s age, weight, and condition. Information like the amount of Meperidine swallowed and at what time would be extremely helpful as well.

Demerol Withdrawal: Symptoms and Timeline
The severity and duration of withdrawal symptoms may vary from person to person due to individual factors. It would largely depend on one’s history of use, misuse, or abuse. Because Meperidine has a short half-life and duration of action, some users have reported early withdrawal symptoms like headaches and anxiety only a few hours after cessation.
Withdrawal Symptoms Can Include the Following:
- Chills
- Anxiety
- Irritability
- Excessive yawning
- Excessive sweating
- Restlessness
- Anxiety
- Paranoia
- Anorexia
- Nausea
- Vomiting
- Diarrhea
- Muscle and bone pain in different parts of the body
- High blood pressure
- Increased heart or respiratory rate
- Runny nose/nasal mucus fluid discharge
- Dilated pupil
- Fever
- Tremors
- Insomnia
Meperidine is a dangerous drug to just suddenly withdraw from. One should seek help and work with a doctor in developing a withdrawal plan or taper schedule to decrease their risk of experiencing severe symptoms. If they are already experiencing symptoms, call the doctor right away for help with proper withdrawal management.
How Long Does Demerol Stay In The System?
Meperidine has a plasma elimination half-life of about 3 to 8 hours in individuals with optimum health. Meanwhile, Normeperidine, its lone bioactive metabolite, has a longer elimination half-life ranging from 8 to 21 hours. Note that in patients with underlying conditions such as hepatic and renal impairment, the elimination half-life may be prolonged.
Meperidine Has a Rapid Onset of Action, Too, With Peak Analgesia Usually Occurring Within the Following Periods:
- 1 hour after oral administration
- 40 minutes to an hour after subcutaneous injection
- 30 to 50 minutes after intramuscular injection
Meperidine shows up on 12-panel drug tests. Detection windows vary for different tests and are highly dependent on one’s metabolism, dose, and frequency of use.
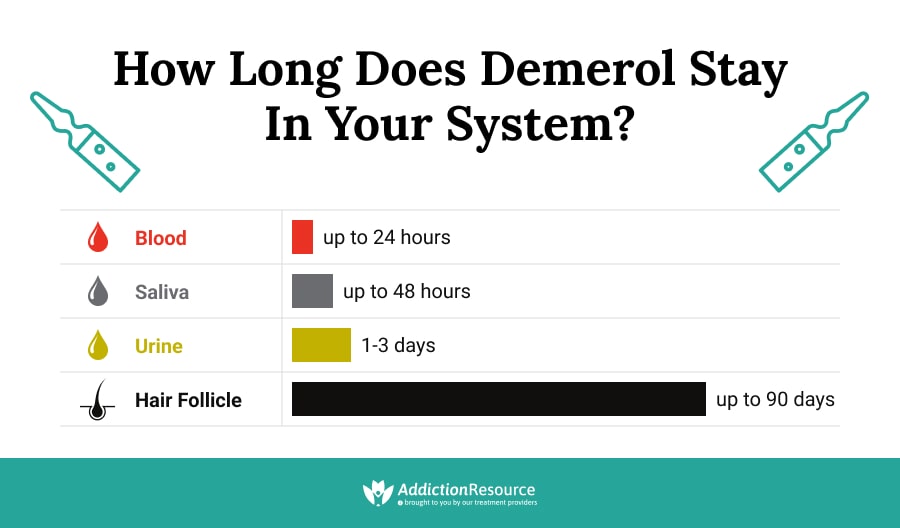
Below Detection Windows for the Most Common Tests:
- Urine – one to three days after last use
- Blood – up to 24 hours after last use
- Saliva – up to 48 hours after last use
- Hair – up to 90 days after last use
- Oral fluid panels – 1 day (with a cut-off level of 5ng/mL)
Demerol Addiction Treatment
The first step toward Demerol addiction recovery is detoxification. It first starts in a hospital or other specialized clinics under medical supervision where a patient’s vital signs will regularly be monitored by a doctor or other medical professionals. Abrupt discontinuation and rapid tapering of Meperidine pose serious risks of severe withdrawal symptoms and pain, and therefore should not be done. To avoid potentially life-threatening withdrawal symptoms and for addiction treatment to be successful, the dosage is gradually reduced with the specifics depending on a patient’s physical and psychological attributes, as well as vital information like the length of time they were under Meperidine treatment, and the dosage they have been using. It is crucial to adjust treatment plans based on how an individual responds so as to fit their changing needs. They must also be closely monitored especially during the initiation (within 24 to 72 hours) of therapy.
A doctor or medical professional may sometimes use other medications such as Naltrexone and Methadone to ease unpleasant withdrawal symptoms. Once a person finishes detox, they can sign into an inpatient rehab facility to make maintaining sobriety easier. Mental health support may also be put in place prior to or during the treatment to help them learn new, functional ways of dealing with everyday issues. Being surrounded by encouraging, loving, and supportive people like family members and friends can also play a huge role in a person’s recovery.
Hope Without Commitment
Find the best treatment options. Call our free and confidential helpline
Most private insurances accepted
Find Drug Rehabilitation Centers Near You Anywhere In the US
Addiction Resource team has compiled an extensive list of the top drug rehabilitation facilities around the country. Use our locator tool to find the best centers near you.
Page Sources
- American Society of Health-System Pharmacists, Inc. (2021, February 25). Meperidine. From MedlinePlus: https://medlineplus.gov/druginfo/meds/a682117.html
- averhealth. (2019). Michigan DHHS Implementation Training Packet. From Michigan Department of Health & Human Services: https://courts.michigan.gov/Administration/SCAO/OfficesPrograms/CWS/Documents/MDHHS_Training_Packet_FINAL.pdf
- Berger, A. (2019, October 12). Opioid Analgesics. From Stanford University: https://med.stanford.edu/content/dam/sm/pedsanesthesia/documents/opioid-analgesics.pdf
- Borke, J. (2019, October 3). Meperidine hydrochloride overdose. From MedlinePlus: https://medlineplus.gov/ency/article/002676.htm
- Centers for Disease Control and Prevention. (2021, March 10). Opioid Overdose Data Analysis and Resources. From Centers for Disease Control and Prevention: https://www.cdc.gov/drugoverdose/data/analysis.html
- Centers for Disease Control and Prevention. (2021, March 25). Opioid Overdose: Synthetic Opioid Overdose. From Centers for Disease Control and Prevention: https://www.cdc.gov/drugoverdose/data/synthetic/index.html
- DailyMed. (2021, April 5). DEMEROL- meperidine hydrochloride injection, solution. From DailyMed: https://dailymed.nlm.nih.gov/dailymed/drugInfo.cfm?setid=b31d1308-28c3-43f4-e0a6-2f3ed76b8975#section-2
- DailyMed. (2021, March 31). DEMEROL- meperidine hydrochloride tablet. From DailyMed: https://dailymed.nlm.nih.gov/dailymed/drugInfo.cfm?setid=5cb2674c-a70d-4022-9188-3f711cccff5e&audience=consumer#section-3
- DEA Diversion Control Division. (n.d.). Controlled Substance Schedules. From U.S. DEPARTMENT OF JUSTICE • DRUG ENFORCEMENT ADMINISTRATION • Diversion Control Division: https://www.deadiversion.usdoj.gov/schedules/
- Drug Enforcement Administration, U.S. Department of Justice. (2020). Drugs of Abuse: A DEA Resource Guide / 2020 Edition. From Get Smart About Drugs: https://www.getsmartaboutdrugs.gov/sites/getsmartaboutdrugs.com/files/publications/Drugs%20of%20Abuse%202020-Web%20Version-508%20compliant.pdf
- Genetics Home Reference. (2017, November 1). Opioid addiction. From MedlinePlus: https://medlineplus.gov/genetics/condition/opioid-addiction/
- McCarthy, D., Murray, S., Galagan, D., Gern, J., & Hutson, P. (1998). Meperidine Attenuates the Secretion but Not the Transcription of IL-1ß in Human Mononuclear Leukocytes. College of Nursing Faculty Research and Publications, 226. From https://epublications.marquette.edu/nursing_fac/226/
- NIDA. (2018, June 6). Understanding Drug Use and Addiction DrugFacts. From National Institute on Drug Abuse: https://www.drugabuse.gov/publications/drugfacts/understanding-drug-use-addiction
- NIDA. (2019, August 5). Genetics and Epigenetics of Addiction DrugFacts. From National Institute on Drug Abuse: https://www.drugabuse.gov/publications/drugfacts/genetics-epigenetics-addiction
- NIDA. (2021, April 13). What classes of prescription drugs are commonly misused? From National Institute on Drug Abuse: https://www.drugabuse.gov/publications/research-reports/misuse-prescription-drugs/what-classes-prescription-drugs-are-commonly-misused
- Tulane University School of Medicine. (2016, April 18). Meperidine. From Tulane University School of Medicine: https://tmedweb.tulane.edu/pharmwiki/doku.php/meperidine?do=
- U.S. Food and Drug Administration. (2010, September). Demerol® (meperidine hydrochloride, USP) . From U.S. Food and Drug Administration: https://www.accessdata.fda.gov/drugsatfda_docs/label/2011/005010s050lbl.pdf
- U.S. Food and Drug Administration. (2017, August). HIGHLIGHTS OF PRESCRIBING INFORMATION . From U.S. Food and Drug Administration: https://www.accessdata.fda.gov/drugsatfda_docs/label/2017/005010s055lbl.pdf


 Reviewed by:
Reviewed by:  Written by:
Written by: 


 FindTreatment.gov
FindTreatment.gov