
Inpatient drug rehab provides a highly structured environment where individuals receive round-the-clock care to overcome substance use disorders. These programs offer a controlled setting with 24/7 medical and therapeutic support, addressing both addiction and underlying mental health conditions to promote lasting recovery. Inpatient rehab also offers evidence-based therapies to address addiction and co-occurring mental health conditions.
According to Statista, in 2023, the US had approximately 28,900 facilities offering addiction treatment, including both inpatient and outpatient options, with 17,561 facilities providing substance use treatment and 12,012 facilities offering mental health treatment. With rising addiction rates, the need for comprehensive addiction rehab programs continues to grow, offering individuals a safe and controlled environment for recovery.
Main inpatient rehab programs include medical detox, dual diagnosis treatment, behavioral therapies, and relapse prevention strategies. Patients also transition into outpatient programs or partial hospitalization programs (PHP) after inpatient care, ensuring continued support in their recovery journey.
The cost of inpatient drug rehab varies widely based on factors like facility type, location, and treatment length. Standard addiction rehab programs range from $5,000 to $20,000 per month, with luxury rehabs exceeding $50,000. Many facilities accept insurance or offer financial assistance to make treatment accessible.
What is the Definition of Inpatient Drug Rehab?
Inpatient drug rehab is a structured, residential treatment program where individuals stay at a specialized facility to receive intensive care for substance addiction. It provides 24/7 medical supervision, therapy, and support to help individuals achieve sobriety. According to the National Institute on Drug Abuse (NIDA), inpatient rehab is particularly effective for severe addiction cases, with studies showing that long-term residential treatment improves recovery outcomes. Programs last from 30 to 90 days, depending on the severity of addiction and individual needs, offering a controlled environment free from triggers and distractions.
What Is a Typical Day in Inpatient Drug Rehab?
A typical day in inpatient drug rehab is highly structured, designed to provide a balanced routine that promotes recovery, stability, and personal growth. The schedule includes medical care, therapy, group activities, and wellness practices to help individuals develop coping skills and maintain long-term sobriety.
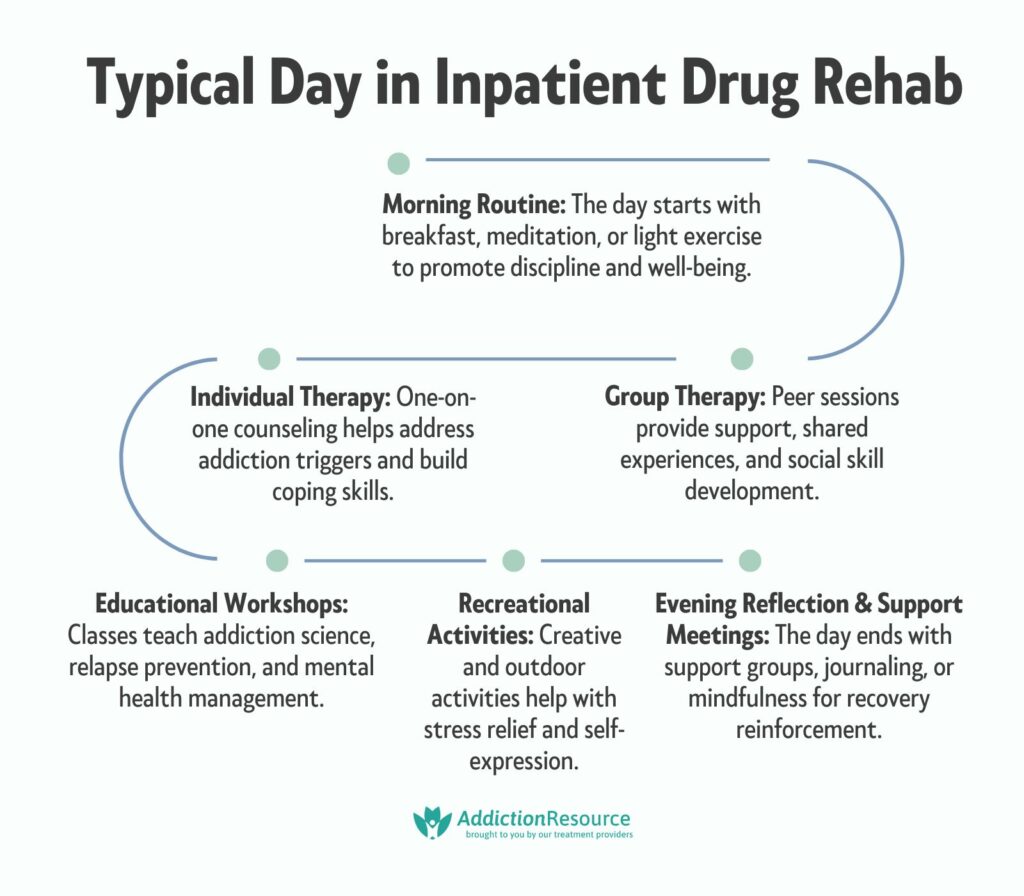
A typical day in inpatient drug rehab is as follows:
- Morning Routine: The day starts early with a healthy breakfast, followed by meditation, yoga, or light exercise. Establishing a structured morning routine helps individuals develop discipline and sets a positive tone for the day.
- Individual Therapy: One-on-one counseling sessions with a licensed therapist help individuals explore underlying causes of addiction, develop coping mechanisms, and set personal recovery goals. Cognitive Behavioral Therapy (CBT) and Motivational Interviewing (MI) are widely used approaches.
- Group Therapy: Peer support is a key component of recovery, and group therapy sessions allow individuals to share experiences, gain encouragement, and develop social skills. These sessions follow a 12-step model or other evidence-based approaches.
- Educational Workshops: Patients attend classes on addiction science, relapse prevention, and mental health education. These workshops help individuals understand the impact of substance use and equip them with tools to manage cravings and stress.
- Recreational Activities: Many rehab centers offer art therapy, music therapy, or outdoor activities such as hiking and sports. These activities provide healthy outlets for self-expression and stress relief.
- Evening Reflection and Support Meetings: Patients participate in support group meetings, such as Narcotics Anonymous (NA) or Alcoholics Anonymous (AA), in the evening. The day concludes with personal reflection, journaling, or mindfulness exercises to reinforce progress.
What Are Different Types of Inpatient Drug Rehab?
Different types of inpatient drug rehab include residential rehab, luxury rehab, dual diagnosis rehab and specialty rehabs that are designed to meet the unique needs of individuals struggling with addiction. These programs vary in structure, treatment approaches, and specialized care options to provide the most effective recovery experience. Choosing the right rehab depends on factors such as co-occurring mental health disorders, personal beliefs, demographics, and professional obligations.
Different types of inpatient drug rehab are as follows:
Residential Rehab
Residential rehab provides a structured, 24/7 treatment environment where individuals live on-site and receive intensive therapy. This type of program focuses on removing external triggers and providing medical and psychological support. According to the National Institute on Drug Abuse (NIDA), residential treatment is highly effective for long-term recovery, with longer stays associated with better outcomes. According to Statista, in 2023, the US had approximately 28,900 facilities offering addiction treatment, including both inpatient and outpatient options.
Dual Diagnosis Rehab
Dual diagnosis rehab is designed for individuals who struggle with both substance use disorder and co-occurring mental health conditions such as depression, anxiety, or PTSD. These programs integrate psychiatric care with addiction treatment, ensuring that both disorders are treated simultaneously. Research from the Substance Abuse and Mental Health Services Administration (SAMHSA) indicates that integrated treatment leads to improved recovery success and lower relapse rates. Overall, 49.9% of all U.S. substance abuse treatment facilities offered dual diagnosis programs/groups, as reported by Mojtabai R. et al. 2004, titled “Which substance abuse treatment facilities offer dual diagnosis programs?”
Luxury Rehab
Luxury rehab offers high-end accommodations and holistic treatment options, including spa treatments, gourmet meals, and private therapy sessions. These facilities cater to individuals preferring a more comfortable and private rehabilitation experience. A study National Drug Helpline. Substance Abuse Hotline found that personalized treatment approaches, found in luxury rehabs, enhance engagement and long-term recovery and cost ranging from $5,000 to $80,000.
Faith-Based Rehab
Faith-based rehab programs incorporate religious or spiritual principles into addiction treatment. These programs use scripture-based teachings, pastoral counseling, and faith-centered support groups such as Celebrate Recovery. Research from the American Journal on Addictions by Yeung JWK. et al. 2022, titled “Faith-based intervention, change of religiosity, and abstinence of substance addicts,” suggests that faith-based treatment is particularly effective for individuals who draw strength from their religious beliefs.
LGBTQ Rehab
LGBTQ rehab provides a safe and supportive environment tailored to the unique challenges faced by LGBTQ individuals in addiction recovery. These programs address issues such as discrimination, identity struggles, and higher rates of substance use in LGBTQ populations. Studies published by the National Institute on Alcohol Abuse and Alcoholism (NIAAA) highlight that LGBTQ individuals benefit from specialized treatment programs that address minority stress factors. In 2022, between 26.5% and 32.3% of lesbian and bisexual women were diagnosed with substance use disorder, compared to about 14% of straight women, according to the Substance Abuse and Mental Health Services Administration (2023).
Teen or Adolescent Rehab
Teen or adolescent rehab programs focus on the specific needs of young individuals struggling with substance use. These programs provide age-appropriate therapy, family counseling, and academic support to help teens recover while continuing their education. The National Center for Biotechnology Information (NCBI) reports that early intervention in adolescence significantly reduces the risk of lifelong addiction. According to NIDA, in the U.S. in 2022, 160 residential addiction treatment centers served adolescents under 18, with only 57% accepting Medicaid, an average wait time of 28 days for a bed, and treatment costs averaging $878 per day.
Rehab for Professionals
Rehab for professionals is designed for working individuals such as doctors, lawyers, executives, and first responders who need addiction treatment while maintaining their careers. These programs offer confidential treatment, flexible schedules, and work-related support. According to the American Medical Association (AMA), professional rehab programs improve recovery outcomes by addressing job-related stressors and maintaining career stability.
Are There Rehabs for Men Only?
Yes, there are rehabs for men only. These facilities provide gender-specific treatment programs tailored to the unique psychological, social, and biological factors that influence substance use in men. Research suggests that men face different triggers and coping mechanisms than women, making specialized treatment beneficial for long-term recovery.
Are There Rehabs for Women Only?
Yes, there are rehabs for women only. Women-specific rehab centers address unique challenges such as trauma, pregnancy, childcare responsibilities, and co-occurring disorders like anxiety and depression. A study by Boyd G et al. 2024, titled “ Exploring Gender Differences in Substance Abuse and Recovery,” indicates that women have different substance use patterns and recovery needs, making gender-specific treatment an effective approach.
What Programs Are Offered in Inpatient Rehab?
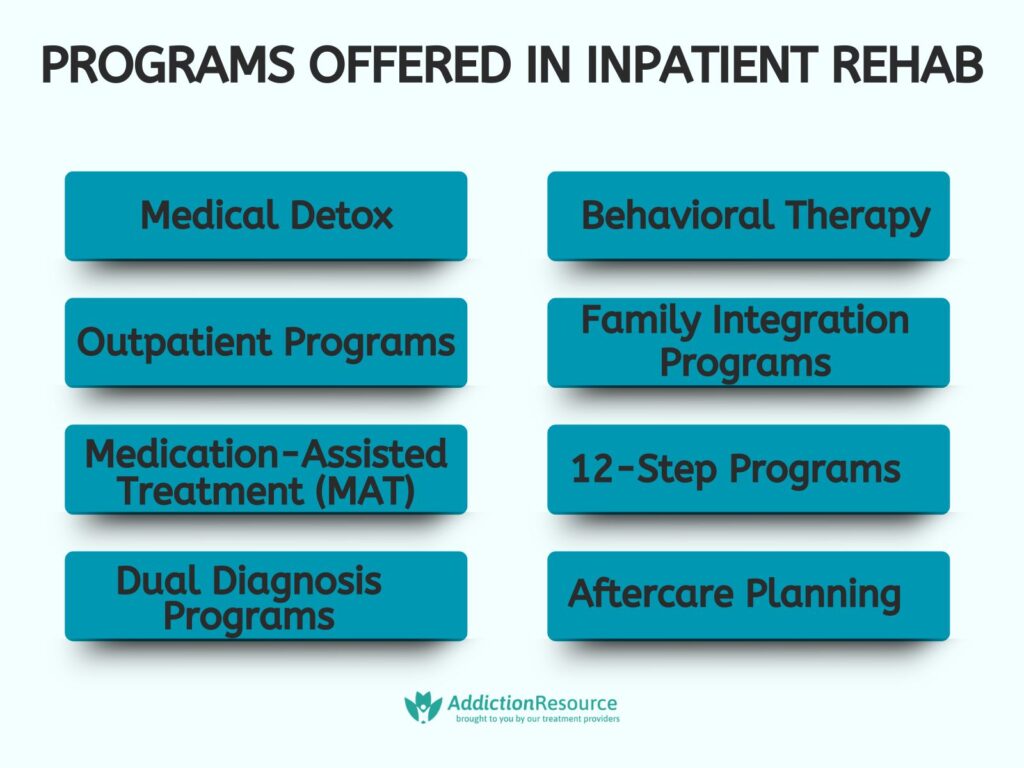
Programs offered in inpatient rehab are medical detox, behavioral therapy, outpatient care, family involvement, medication-assisted treatment (MAT), 12-step programs, intensive outpatient programs, dual diagnosis treatment, and aftercare planning. Each program plays a necessary role in ensuring long-term recovery and relapse prevention.
The following programs are offered in inpatient rehab:
Medical Detox
Medical detox is the first step in inpatient rehab, helping individuals safely withdraw from substances such as alcohol, opioids, and benzodiazepines. This process is medically supervised to manage withdrawal symptoms and prevent complications, which are sometimes life-threatening. For example, withdrawal from alcohol and benzodiazepines leads to seizures if not managed properly. According to the National Institute on Drug Abuse (NIDA), detox alone is not a complete treatment but is necessary for preparing individuals for further therapy. Once the body is free from substances through detox, patients engage in therapy and counseling to address the underlying causes of addiction.
Behavioral Therapy
Behavioral therapy is a core component of inpatient rehab, helping individuals identify and change negative thought patterns and behaviors related to substance use. There are various types of behavioral therapies used in addiction treatment.
The following are the behavioral therapies done in the inpatient drug rehab:
- Cognitive-Behavioral Therapy (CBT): CBT is based on the principle that maladaptive thought patterns contribute to substance use. It helps individuals identify and reframe cognitive distortions, develop problem-solving skills, and implement behavioral strategies such as stimulus control and coping skills training. A study by McHugh RK, Hearon BA, and Otto M.W. et al. 2010, titled “Cognitive behavioral therapy for substance use disorders” indicates that CBT enhances self-efficacy and significantly reduces the likelihood of relapse by reinforcing alternative behaviors to substance use.
- Dialectical Behavior Therapy (DBT): Originally developed for borderline personality disorder, DBT is highly effective for individuals with co-occurring substance use and emotional dysregulation issues. It integrates mindfulness, distress tolerance, emotional regulation, and interpersonal effectiveness techniques to help individuals manage urges and tolerate discomfort without resorting to substance use. Research by Dimeff LA, Linehan MM. et al. 2008, titled “Dialectical behavior therapy for substance abusers,” has demonstrated that DBT reduces impulsivity, enhances emotional stability, and decreases substance dependence.
- Motivational Interviewing (MI): MI is a client-centered, evidence-based approach designed to enhance motivation for change by resolving ambivalence toward substance use. It operates on principles of autonomy, collaboration, and evocation, helping individuals identify their personal reasons for recovery. A neuroimaging study by Parvaz MA, et al. 2011, titled “Neuroimaging for drug addiction and related behaviors” suggests that MI activates brain regions associated with decision-making and goal-directed behavior, reinforcing long-term commitment to sobriety.
- Contingency Management (CM): CM is a behavioral intervention based on operant conditioning principles, where positive reinforcement (such as monetary vouchers or privileges) is provided for drug-free urine samples or treatment adherence. Research, including randomized controlled trial by Ginley MK, Pfund RA, Rash CJ, Zajac K. et al. 2021, titled “Long-term efficacy of contingency management treatment based on objective indicators of abstinence from illicit substance use up to 1 year following treatment: A meta-analysis,” has shown that CM significantly increases abstinence rates, particularly for stimulant and opioid use disorders, by strengthening the brain’s reward system in ways that counteract drug-related reinforcement.
Outpatient Programs
Outpatient programs provide structured treatment while allowing individuals to live at home, making them ideal for those transitioning from inpatient rehab.
There are the following different levels of outpatient care:
- Partial Hospitalization Programs (PHP): PHPs provide structured, intensive treatment for individuals who need high care but do not require 24-hour supervision. Patients attend therapy for 4 to 8 hours daily, 5 to 7 days weekly. Treatment includes medical monitoring, individual and group therapy, and medication management. Studies indicate that PHPs are particularly effective for individuals with co-occurring mental health disorders as they provide comprehensive psychiatric care alongside addiction treatment.
- Intensive Outpatient Programs (IOP): IOPs offer a structured level of care that involves 9 to 20 hours of treatment per week. They balance intensive therapy and the flexibility to maintain daily responsibilities. Research by McCarty, D., et al. 2014, titled “Substance abuse intensive outpatient programs: Assessing the evidence,” shows that IOPs are effective for individuals transitioning from inpatient rehab or PHPs, as they reinforce relapse prevention strategies and offer continued support. Neurobiological studies suggest that sustained engagement in IOPs helps regulate stress-response systems, reducing the likelihood of relapse.
- Standard Outpatient Programs (OP): OPs involve weekly therapy sessions, peer support groups (such as 12-step meetings), and occasional medication management. These programs are best suited for individuals with mild to moderate substance use disorders who have a stable home environment. A study by McKay JR. et al. 2021, titled “Impact of Continuing Care on Recovery From Substance Use Disorder,” indicate that long-term outpatient care is required for sustaining recovery, as it reinforces behavioral changes, provides accountability, and helps individuals integrate coping strategies into their daily lives.
Family Integration Programs
Family integration programs involve loved ones in recovery to strengthen support systems. These programs address family dynamics, communication patterns, and codependency issues that contribute to addiction.
Common components of family therapy include:
- Education on Addiction: Family therapy provides evidence-based education on the neurobiology of addiction, explaining how substance use disorders (SUDs) alter brain function, particularly in areas related to decision-making, impulse control, and reward processing. Research from the National Institute on Drug Abuse (NIDA) highlights that when families understand addiction as a chronic brain disorder rather than a moral failing, they are more likely to offer supportive and nonjudgmental assistance, leading to better treatment engagement and recovery outcomes.
- Communication Skills Training: Effective communication is important for reducing stress, preventing misunderstandings, and encouraging a supportive home environment. Family therapy teaches active listening, assertiveness, and non-confrontational dialogue techniques. A study by Xia Y et al. 2022, titled “Family Function Impacts Relapse Tendency in Substance Use Disorder: Mediated Through Self-Esteem and Resilience,” in addiction psychology suggests that improving family communication reduces relapse risk by lowering emotional distress and preventing enabling behaviors, which inadvertently reinforce substance use.
- Boundary Setting: Establishing healthy boundaries is important for preventing codependency and ensuring accountability in recovery. This involves distinguishing between supportive behaviors (e.g., encouraging treatment) and enabling behaviors (e.g., covering up consequences of substance use). Research indicates that structured family dynamics with clear expectations and consequences help reduce the likelihood of relapse by promoting self-efficacy and personal responsibility in individuals recovering from addiction.
Medication-Assisted Treatment (MAT)
Medication-Assisted Treatment (MAT) combines FDA-approved medications with therapy to treat opioid and alcohol addiction. MAT helps reduce cravings, prevent withdrawal symptoms, and lower the risk of relapse.
Common medications used in MAT include:
- Buprenorphine (Suboxone): Buprenorphine is a partial opioid agonist that binds to opioid receptors, reducing cravings and withdrawal symptoms without producing the same high as full opioids. It has a ceiling effect, meaning its effects level off at higher doses, lowering the risk of misuse and overdose. A study by Shulman M, Wai JM, Nunes EV. et al. 2019, titled “Buprenorphine Treatment for Opioid Use Disorder: An Overview,” indicate that buprenorphine treatment significantly improves retention in opioid use disorder (OUD) treatment and reduces illicit opioid use.
- Methadone: Methadone is a full opioid agonist that activates opioid receptors more gradually than drugs like heroin or fentanyl, helping to prevent withdrawal and reduce cravings without inducing euphoria when taken as prescribed. It has been used for decades in Medication-Assisted Treatment (MAT) and is regulated through specialized clinics. Research from the National Institute on Drug Abuse (NIDA) shows that patients receiving methadone maintenance treatment have lower rates of overdose, criminal activity, and infectious disease transmission compared to those who attempt abstinence without medication.
- Naltrexone (Vivitrol): Naltrexone is an opioid antagonist, meaning it blocks opioid receptors, preventing opioids from producing pleasurable effects. Unlike buprenorphine and methadone, it does not activate the receptors at all, making it a non-addictive option. Studies in the Journal of the American Medical Association (JAMA) suggest that extended-release naltrexone significantly reduces relapse rates in both opioid and alcohol use disorders. However, adherence is a challenge since individuals must be fully detoxed before starting treatment.
- Acamprosate (Campral): Acamprosate helps restore neurotransmitter balance in the brain, particularly in the glutamate and GABA systems, which are disrupted by chronic alcohol use. It reduces withdrawal symptoms such as anxiety, insomnia, and restlessness, making it easier for individuals to maintain abstinence. Clinical trial by Feeney GF, Connor JP, Young RM, Tucker J, McPherson A. et al. 2006, titled “Combined acamprosate and naltrexone, with cognitive behavioural therapy is superior to either medication alone for alcohol abstinence: a single centres’ experience with pharmacotherapy,” have demonstrated that acamprosate improves alcohol abstinence rates, especially when combined with behavioral therapy.
12-Step Programs
12-step programs, such as Alcoholics Anonymous (AA) and Narcotics Anonymous (NA), provide peer support and a structured framework for maintaining sobriety. Individuals who regularly attend 12-step meetings have higher long-term sobriety rates. The peer support and accountability provided by these groups help individuals stay committed to their recovery journey.
The 12-step programs include:
- Admitting powerlessness over addiction.
- Seeking help from a higher power (as personally defined).
- Making amends for past mistakes.
- Continuing personal growth and service to others.
Dual Diagnosis Programs
Dual diagnosis programs treat individuals with both a substance use disorder and a co-occurring mental health condition, such as depression, anxiety, or PTSD. This integrated approach is important because untreated mental health conditions contribute to addiction and relapse.
Treatment in a dual diagnosis program includes:
- Psychiatric Care: Dual diagnosis programs provide comprehensive psychiatric care, including medication management for mental health disorders such as depression, anxiety, bipolar disorder, and schizophrenia. Medications like selective serotonin reuptake inhibitors (SSRIs) for depression or mood stabilizers for bipolar disorder are prescribed alongside substance use treatment. Research by Yule AM, Kelly JF. et al. 2019, titled “Integrating Treatment for Co-Occurring Mental Health Conditions,” suggests that integrated psychiatric care significantly improves treatment adherence and reduces relapse rates by addressing both disorders concurrently rather than separately.
- Therapy: Evidence-based therapies such as Cognitive-Behavioral Therapy (CBT), Dialectical Behavior Therapy (DBT), and trauma-focused therapies help individuals understand the link between mental health and substance use. CBT helps individuals reframe negative thought patterns contributing to substance use, while DBT improves emotional regulation and distress tolerance. Trauma-focused therapies, such as Eye Movement Desensitization and Reprocessing (EMDR), are beneficial for individuals with post-traumatic stress disorder (PTSD) and co-occurring substance use disorders.
- Holistic Treatments: Many dual diagnosis programs incorporate holistic treatments like mindfulness meditation, yoga, and acupuncture to reduce stress, improve emotional well-being, and promote recovery. Research by Sancho M et al. 2018, titled ”Mindfulness-Based Interventions for the Treatment of Substance and Behavioral Addictions: A Systematic Review,” suggests that mindfulness-based interventions decrease substance cravings and improve mental health symptoms by enhancing self-awareness and emotional regulation. Yoga and meditation have also been shown to lower cortisol levels, reducing stress-related relapse risks.
Aftercare Planning
Aftercare planning ensures that individuals have a structured recovery plan post-rehab, including continued therapy, support groups, and relapse prevention strategies.
Common components of aftercare include:
- Sober Living Homes: Sober living homes provide a structured, drug-free environment where individuals in recovery transition from inpatient treatment to independent living. These residences promote accountability through house rules, mandatory drug testing, and peer support. Research published in the Journal of Psychoactive Drugs found that individuals who stay in sober living homes for at least 6 months have lower relapse rates and improved social functioning compared to those who transition directly to unsupervised living. The structured yet flexible environment helps residents maintain sobriety while reintegrating into daily life.
- Ongoing Therapy: Continued therapy, including Cognitive-Behavioral Therapy (CBT), Motivational Interviewing (MI), and trauma-focused counseling, helps individuals identify and manage triggers that lead to relapse. Regular one-on-one or group therapy sessions provide emotional support, reinforce coping strategies, and help maintain progress. A study by Guenzel N, McChargue D. et al. 2023, titled “Addiction Relapse Prevention,” found that ongoing therapy reduces the likelihood of relapse by improving emotional regulation and strengthening problem-solving skills.
- Support Groups: Participation in 12-step programs like Alcoholics Anonymous (AA) or Narcotics Anonymous (NA), as well as non-12-step alternatives such as SMART Recovery, provides peer support and accountability. Regular attendance in support groups significantly increases the chances of long-term sobriety. Support groups help individuals stay motivated, share experiences, and develop a sense of community, reducing feelings of isolation that contribute to relapse.
- Employment and Life Skills Training: Many aftercare programs include vocational training, financial management, and other life skills to help individuals rebuild their lives after rehab. Employment assistance programs teach job-seeking strategies, resume-building skills, and workplace readiness. A report from the Substance Abuse and Mental Health Services Administration (SAMHSA) highlights that individuals who secure stable employment after treatment are more likely to maintain long-term sobriety and experience improved mental health outcomes.
What Medications are Used During Inpatient Rehab?
Medications used during inpatient rehab are prescribed to help manage withdrawal symptoms, reduce cravings, and prevent relapse for individuals recovering from substance use disorders. These medications vary depending on the substance being treated and are combined with behavioral therapies for a comprehensive approach to recovery. Medical supervision ensures that medications are used safely and effectively to support long-term sobriety.
Common medications used in inpatient rehab are as follows:
- Buprenorphine: Buprenorphine is used to treat opioid addiction. It is a partial opioid agonist that reduces withdrawal symptoms and cravings without producing the same high as other opioids. It is combined with naloxone (as in Suboxone) to deter misuse. Research from the National Institute on Drug Abuse (NIDA) shows that buprenorphine significantly reduces opioid relapse rates.
- Methadone: Methadone is a long-acting opioid agonist used for opioid addiction. Methadone prevents withdrawal symptoms and cravings by stabilizing brain chemistry. It is used in medication-assisted treatment (MAT) and requires close medical supervision due to its potential for dependence. A study by Mattick RP, Breen C, Kimber J, and Davoli M. Methadone maintenance therapy versus no opioid replacement therapy for opioid dependence,” have shown that methadone maintenance therapy improves retention in treatment and reduces illicit opioid use.
- Naltrexone: Naltrexone is used for both opioid and alcohol addiction. Naltrexone is an opioid antagonist that blocks the euphoric effects of opioids and alcohol. Unlike buprenorphine and methadone, it does not cause physical dependence. According to SAMHSA, naltrexone is most effective when combined with counseling and behavioral therapy.
- Acamprosate: Acamprosate is primarily used to treat alcohol use disorder. Acamprosate helps individuals maintain abstinence by stabilizing brain chemistry disrupted by chronic alcohol use. Clinical study by Yahn SL, Watterson LR, Olive MF. et al. 2013, titled “Safety and efficacy of acamprosate for the treatment of alcohol dependence” indicate that acamprosate improves long-term recovery outcomes when used alongside therapy. The study found a reduced risk of returning to any drinking after detoxification by 86% and increased the sum of days a patient remained abstinent during the study by 11%.
- Disulfiram: Disulfiram is a medication for alcohol addiction. It causes unpleasant reactions (such as nausea, vomiting, and flushing) when alcohol is consumed. It acts as a deterrent for individuals trying to remain sober. Studies have found that disulfiram is most effective when combined with behavioral support and regular monitoring.
- Benzodiazepines: Benzodiazepines are used during alcohol or benzodiazepine withdrawal. These medications help manage severe withdrawal symptoms such as seizures and anxiety. They are prescribed for short-term use under strict medical supervision due to their potential for dependence.
- Antidepressants: For individuals with co-occurring mental health disorders, antidepressants are prescribed to manage depression and anxiety, which are common during recovery. Treating underlying mental health conditions improves overall treatment success.
- Antipsychotics: Used for patients with co-occurring schizophrenia, bipolar disorder, or other severe psychiatric conditions, antipsychotic medications help regulate mood and prevent psychotic symptoms, which are exacerbated by substance use.
Does Inpatient Drug Rehab Treat Dual Diagnosis Disorders?
Yes, inpatient drug rehab does treat dual-diagnosis disorders. Dual diagnosis treatment addresses co-occurring disorders, where a person experiences both a substance use disorder and a mental health condition, such as depression, anxiety, or PTSD. Inpatient rehab provides integrated care, including psychiatric evaluation, medication management, and evidence-based therapies like Cognitive-Behavioral Therapy (CBT) and Dialectical Behavior Therapy (DBT). Research by HelpGuide.org shows that treating both conditions simultaneously leads to better long-term recovery outcomes, reducing relapse risk and improving mental health stability.
How Much Does Inpatient Rehab Cost?
The cost of inpatient drug rehabilitation on average cost between $20,000 and $35,000 for a 30-day program. The cost varies widely based on factors such as the type of facility, level of care, and geographic location. Luxury or executive facilities, offering high-end amenities and personalized services, charge significantly more, with prices reaching $80,000 or higher per month.
The cost of inpatient rehab ranges based on the type of inpatient treatment as follows:
| Type of Facility | Average Monthly Cost |
| Standard Inpatient Rehab | $20,000 – $35,000 |
| Luxury Inpatient Rehab | $50,000 – $80,000+ |
The cost of inpatient rehab also varies by state due to differences in the cost of living, state regulations, and the availability of facilities. For example, treatment centers in states like California and New York, where the cost of living is higher, charge more than facilities in states with a lower cost of living. Areas with a higher concentration of luxury rehab centers, such as Malibu, California, have higher average costs.
It’s important to note that these figures are approximate, and actual costs vary based on specific services offered, the length of the program, and individual patient needs. Prospective patients should contact facilities directly to obtain accurate pricing information and inquire about insurance coverage or financing options.
How Does Insurance Work for Rehab Treatment?
Insurance works for rehab treatment by covering part or all of the costs of inpatient and outpatient addiction care, depending on the policy and provider. Most insurance plans, including private insurance, Medicaid, and Medicare, offer some level of coverage for substance use disorder treatment. Coverage varies based on factors such as the type of plan, the state of residence, and whether the rehab facility is in-network or out-of-network. Many insurance providers require pre-authorization and have limits on the duration of stay or types of services covered.
Are There Payment Plans Available for Inpatient Rehab?
Yes, there are payment plans available for inpatient rehab to help patients afford treatment. These plans allow individuals to pay in installments over time rather than upfront. Some rehab centers also provide sliding scale fees, financial assistance programs, or financing options for those without insurance or with limited coverage.
What Factors Affect the Cost of Inpatient Rehab?
Factors affecting the cost of inpatient rehab include the type of facility, length of stay, level of care, and location. Luxury rehabs, extended programs, and high-cost states tend to have higher expenses, while nonprofit or state-funded facilities are more affordable.
The following are the factors affecting the cost of inpatient rehab:
- Type of Facility: Rehab facilities are categorized into standard, luxury, or executive rehab. Each type has a different price range based on the level of services, accommodations, and specialized features available.
- Length of Stay: The overall cost increases with longer treatment durations, as extended stays require more resources, therapy sessions, and medical care.
- Level of Care: Programs that include intensive medical detox, dual diagnosis treatment, or specialized therapies tend to have higher costs due to the need for additional medical supervision and tailored treatment plans.
- Location: Rehabs in states with a high cost of living, such as California and New York, charge more than those in lower-cost regions due to operational expenses and demand.
- Amenities and Services: Luxury rehabs that offer private rooms, holistic therapies, gourmet meals, and personalized treatment options come at a premium cost compared to standard rehab centers.
- Insurance Coverage: The amount an individual pays out-of-pocket depends on their insurance plan, with factors such as deductibles, copayments, and in-network vs. out-of-network coverage affecting overall costs.
- Financial Assistance: Some rehab centers provide sliding scale fees, scholarships, grants, or state-funded programs that help reduce expenses for individuals who qualify for financial aid.
How to Find an Inpatient Drug Rehab Near Me?
To find an inpatient drug rehab near me, you have online resources, the option to consult healthcare professionals, or contact addiction helplines for guidance. Researching facilities for a drug rehab near me, comparing treatment options, and verifying accreditation help ensure you choose the best rehab center for your needs.
Following are the things to look for in an inpatient drug rehab:
- Accreditation and Licensing: Ensure the facility is accredited by organizations like the Joint Commission or CARF to guarantee quality care.
- Treatment Approach: Look for evidence-based treatment programs, such as cognitive-behavioral therapy (CBT), medication-assisted treatment (MAT), or holistic therapies.
- Specialized Programs: Consider facilities offering programs for specific needs, such as dual diagnosis, LGBTQ+ support, or faith-based treatment.
- Insurance and Payment Options: Verify whether the rehab center accepts your insurance and offers financial aid or payment plans if needed.
- Facility Amenities: Evaluate the environment, living conditions, and amenities to ensure comfort and support during recovery.
- Aftercare Services: Look for rehabs that provide ongoing support, such as outpatient programs, relapse prevention, and alumni groups.
What Is the Difference Between Inpatient and Outpatient Drug Rehab?
The difference between inpatient and outpatient drug rehab is that inpatient rehab requires individuals to stay at a treatment facility 24/7, while outpatient rehab allows them to live at home and attend treatment sessions on a scheduled basis. Inpatient rehab is more intensive, providing structured care, while outpatient rehab offers flexibility for those with work, school, or family responsibilities. In general, both inpatient and outpatient treatment have their own strengths and weaknesses, with success rates varying based on individual circumstances and the severity of the condition. Inpatient care offers a more structured, supervised environment, while outpatient rehab allows for maintaining daily life while receiving treatment.
How Long Is Inpatient Drug Rehab?
Inpatient drug rehab lasts 30, 60, or 90 days, though some programs extend beyond 90 days for severe cases. The duration depends on factors such as the type of substance used, the severity of addiction, and whether a dual diagnosis (co-occurring mental health disorder) is present.
Longer programs are recommended for individuals with chronic addiction or multiple relapses. While 30-day programs provide a foundation for recovery, 60- or 90-day programs offer deeper therapeutic interventions and relapse prevention strategies. Some facilities also offer extended residential care for those needing additional support.
What Happens After Inpatient Drug Rehab?
After inpatient drug rehab, individuals transition into ongoing care programs to maintain long-term sobriety and prevent relapse. This phase is important for reinforcing recovery skills and staying connected to a support system. Many individuals continue treatment through outpatient programs, which provide therapy and support while allowing them to live at home. Aftercare services, such as counseling, case management, and relapse prevention planning, help maintain progress. Support groups like Alcoholics Anonymous (AA) or SMART Recovery offer peer support and accountability. Many rehab facilities have alumni programs that provide continued engagement and encouragement. Continuing care is paramount for long-term success, as it helps individuals navigate real-world challenges while staying committed to their sobriety.





 FindTreatment.gov
FindTreatment.gov